CNS shares insight on building multidisciplinary teams
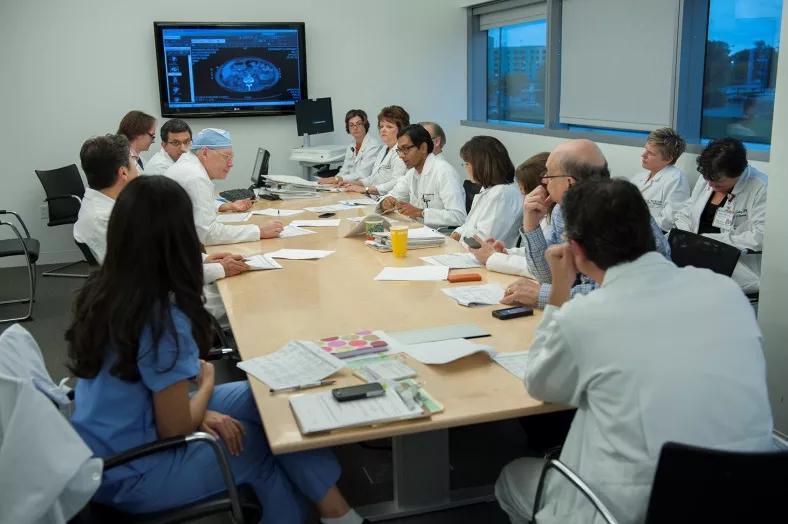
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7e7d77db-d1a7-42a1-89af-49a13eb636fe/16-HRT-294-Inset-1_jpg)
Figure 1. A meeting of the Cleveland Clinic clinical team as they prepared guidance for Saint Francis Medical Center on how to design and launch a TAVR program.
When you ask Deborah Klein, MSN, APRN, ACNS-BC, CCRN, FAHA, FAAN who she teams with as a clinical nurse specialist in the coronary ICU, heart failure ICU and cardiac accelerated recovery/cardiac short-stay/post-anesthesia care at Cleveland Clinic’s main campus, her answer is simple – everyone.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Although we are all here for the same purpose, we each bring a very specific skill set,” she says. “None of us can work in isolation in addressing all of the challenges related to patients, families and the hospital system.”
Klein fosters teamwork among healthcare providers on her units in many ways, ranging from informal one-on-one collaboration to formal multidisciplinary initiatives sanctioned by the Cleveland Clinic healthcare system. The latter includes these two notable initiatives:
Prior to the meeting, Klein and clinical nurses identify long-term patients and patients whose plan of care may be unclear to the group. “As a team, we discuss where we are with those patients and where we are going,” says Klein. “It gets us all on the same page without having to decipher notes in the electronic medical record.” For example, if it looks like a patient is headed toward long-term acute care, the case manager and social worker are on hand and can start the process. If a patient requires alternative medical therapies, the team can sort through the options together, each lending their unique insight.
Advertisement
Since the council began in 2011, it has standardized care using the best evidence around central venous catheters, cardiac assist devices, mechanical ventilation, chest tubes, Foley catheters and more. “One of our greatest accomplishments is standardizing our end-of-life care,” says Klein. “Because there is trust and respect among council members, we can have tough conversations and make decisions based on the best evidence that benefit patients, families and the healthcare team.”
The key to working well together, asserts Klein, is open communication. “Be open in your mind, your body language and the words you use,” she says. “It’s about mutual respect – being able to listen to different viewpoints and trying to understand that person’s frame of reference.”
Klein offers a handful of tips for fostering interprofessional collaboration:
Advertisement
As the healthcare landscape continues to transform, interprofessional collaboration is more important than ever. Says Klein, “Be open to the process.”
Advertisement
Advertisement
Nurses play key role in comprehensive lifetime treatment program
Customized bots improve speed, efficiency by streamlining daily clinical, clerical tasks
Nurses play pivotal role in patients’ ability to recover in the comfort of their own homes
New protocol reduces costs, increases patient and caregiver satisfaction
Advocating for patient safety is imperative in fast-paced surgical settings
M-Power program improves the perinatal experience for people who have survived abuse
Advice for those pursuing a WOC nursing career
Veteran nurse shares his experience as a caregiver and community volunteer