Empowering athletic trainers to better assess, report and monitor head injury

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2b3d216e-9c1a-459c-b0d6-7f8d1c86fe52/16-NEU-2804-C3App-650x450_jpg)
16-NEU-2804-C3App-650×450
When Cleveland Clinic’s Concussion Center introduced its C3Logix™ mobile app for concussion assessment in 2011, a key objective was to guide decision-making around how to evaluate and where to dispatch student athletes in the wake of a blow to the head. Data from the app’s fifth year of use confirm that’s indeed a leading way the app is being employed. This post details those data and shares a few other statistical snapshots as applications of C3Logix continue to evolve.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As detailed in earlier posts on this site, the Cleveland Clinic-developed C3Logix app consists of a battery of tests — given to a student athlete at baseline and following an injury — to help gauge the severity of a suspected concussion. By comparing assessments of balance, reaction time, memory and vision after an injury to baseline and normative data, the app helps determine areas of most concern and guide therapy.
The app’s concussion incident report module allows athletic trainers to collect and report details of head injuries at the time of an incident on an iPad®, iPhone® or other mobile device. Data provided by coaches on the sidelines — e.g., on time of injury, symptoms and action(s) taken — provide invaluable information to physicians in the hospital or office and also can facilitate care collaboration.
As detailed in the bar graph below, baseline and follow-up C3Logix assessments increased dramatically in 2014 and continued at high numbers throughout 2015. Since the app’s introduction in a pilot program in 2011, its use has extended beyond Northeast Ohio, with more than 20,000 high school and college athletes in the country undergoing baseline testing in the fourth quarter of 2015 alone. The Concussion Center is currently analyzing the baseline and post-injury data from these reports.
As shown by the red line in the graph below, incident reports have steadily increased since July 2014, when Cleveland Clinic athletic trainers received education on use of the incident report module, with approximately 2,700 incident reports filed by the fourth quarter of 2015.
Advertisement
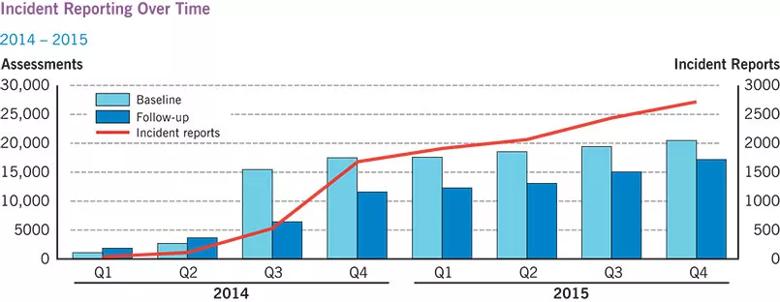
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0f144d32-01b5-4818-8ebe-0d09a44acf15/16-NEU-2804-C3App-Inset1_jpg)
Action taken immediately following a head injury can be critical to prevent more serious injury from a subsequent blow to the head. Incident report data (below) from 232 same-day incident reports in 2015 show that student athletes were usually taken out of action (81.4 percent), by being sent to either the locker room, the sideline, home or for further medical evaluation. In fewer than 5 percent of reported cases did the athlete return to play the same day. Missing data for nearly 14 percent of reports represents an opportunity for improvement in future data collection efforts.
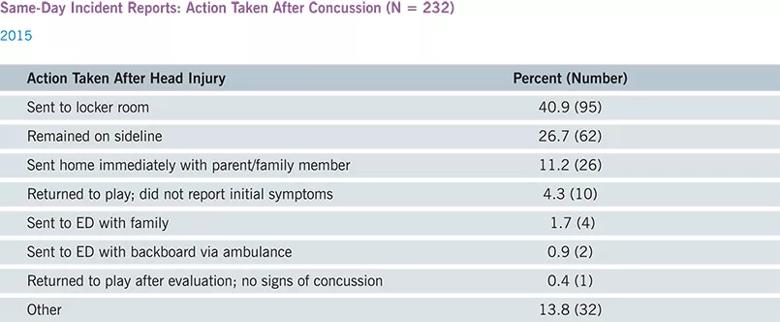
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2666c562-5c72-47bc-81c2-761d4b10ee61/16-NEU-2804-C3App-Inset2_jpg)
The app’s return-to-play (RTP) module allows an athletic trainer to monitor recovery after a concussion, based on a six-phase graduated protocol of increasing exertion recommended by consensus guidelines. The module also allows documentation of missed school days.
In fall 2015, the RTP module was used for 515 student athletes following a head injury, 21 percent of whom missed school, for an average duration of 3.4 days. Such information is useful for providing athletes — as well as teachers, school administrators and counselors — with realistic expectations of recovery time.
Advertisement
Advertisement
New study advances understanding of patient-defined goals
Testing options and therapies are expanding for this poorly understood sleep disorder
Real-world claims data and tissue culture studies set the stage for randomized clinical testing
Digital subtraction angiography remains central to assessment of ‘benign’ PMSAH
Cleveland Clinic neuromuscular specialist shares insights on AI in his field and beyond
Findings challenge dogma that microglia are exclusively destructive regardless of location in brain
Neurology is especially well positioned for opportunities to enhance clinical care and medical training
New review distills insights from studies over the past decade